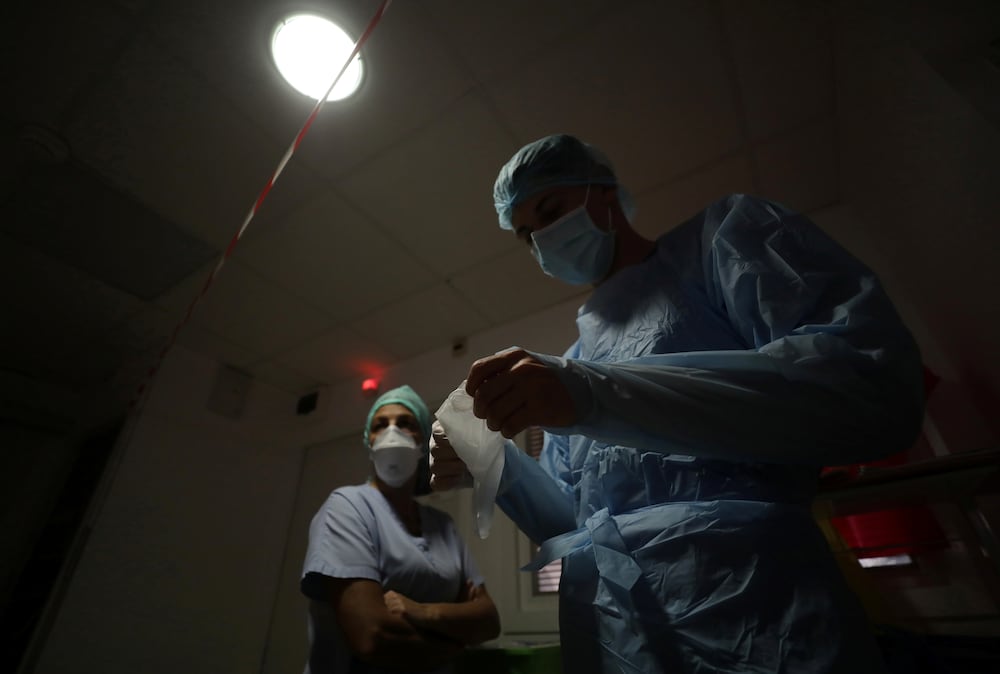
More than 10% of people with severe covid produce a type of antibodies that instead of protecting them from the virus worsens the infection by boycotting their immune system.
It is the result of an international study that can explain why some people experience covid without knowing it or with very mild symptoms while others develop a serious or fatal disease.
Until now, three major risk factors were known: being a man, being older, and having previous illnesses.
The work adds a fourth: congenital genetic defects that can prevent the immune system from fighting and eliminating the virus.
This type of problem seems to be much more common in men than women.
"This finding will change the treatment of some patients," explains Carlos Rodríguez-Gallego, immunologist at the University Hospital of Gran Canaria Doctor Negrín and co-author of the study, which is published today in the journal
Science
.
"Our team is already studying how to establish clinical trials to identify patients who produce these types of autoantibodies and perhaps treat them with other types of antibodies to counteract the problem," he says.
The study has analyzed the blood of almost 1,000 patients with very severe pneumonia caused by the coronavirus and compared it with that of 600 infected asymptomatic or with mild symptoms and with a third group of 1,200 healthy volunteers.
Antibodies that neutralize type 1 interferon, an essential molecule to raise a general alarm when a virus enters our body, were found in 10.2% of critically ill patients.
Minutes after SARS-CoV-2 infects a cell, the first line of defense of our immune system is launched.
When they detect the presence of the virus, the dendritic cells begin to produce a protein that sends an alarm signal to the whole body: interferon 1. These interferons can bind to the cells of almost all the tissues of the body and modify their metabolism so that activate their antiviral defense mechanisms.
Until now, three major risk factors were known: being a man, being older, and having previous illnesses.
The work adds a fourth: congenital genetic defects
What this work has observed is that a percentage of patients have genetic defects that cause them to produce antibodies that, instead of finding and neutralizing the virus, are designed to block interferon 1. The study has found several types of antibodies against interferons in that 10.2% of patients and points out that they are the cause of these patients getting worse until their life is in danger.
"Interferon is so called because it interferes with the multiplication of the virus and stops it," explains Javier Martínez-Picado, ICREA researcher at IrsiCaixa and co-author of the study.
"The autoantibodies produced by these patients sequester interferon and cancel it," he highlights.
In another work also published in
Science,
the same international consortium shows that certain genetic alterations that affect the production of interferon would explain 3.5% of severe cases of covid.
Both works help explain why 14% of infected people end up developing a serious disease that can kill them.
This is the largest study to date on the genetic causes of severe covid, says Martínez-Picado, especially because it demonstrates the action of these autoantibodies.
Scientists have shown that if interferon 1 is added to cells infected with SARS-CoV-2, the infection is paralyzed.
But if you add plasma from patients that produce these autoantibodies, the infection restarts and the viruses continue to make tens of thousands of copies of themselves.
The two jobs can help identify patients at higher risk for life-threatening pneumonia and even search for specific treatments for them.
It is not that the virus activates the production of these negative effect antibodies, but rather that its production is due to innate genetic defects of the immune system.
The presence of these molecules "is a bad omen in the clinical progression of the patient", explains Martínez-Picado.
A very interesting fact is that 95% of the patients who produce these molecules are men.
And this is surprising, since autoimmune diseases are more common in women than in men.
The detection of these antibodies is not routine clinical practice, but it is easy to develop tests that are not very complex to detect them and also genetic analyzes that identify the patients who produce them.
Why are young people without previous ailments who become seriously ill from covid or even die?
This is one of the questions that began the work of the Human Genetics and Covid Project, led by Jean Laurent Casanova, a researcher at the French National Institute for Health and Medicine Research and the Rockefeller University in the USA. Part of the answer may be be in rare genetic defects;
so there may be three patients with the same mutation, one in New York, one in Sydney, and one more in Tokyo.
There may be dozens of genetic defects like these that explain part of the most serious cases and the only way to identify them and establish a pattern is by establishing an international collaboration like this one, explains Casanova on the website of the consortium, made up of hundreds of hospitals that contribute samples. blood samples and genetic sequencing nodes where samples are analyzed.
In Spain, in addition to the Canarian hospital, the Germans Trias i Pujol, Vall d'Hebron hospitals in Barcelona and the Mutua de Terrassa University Hospital, as well as the Idibell and IrsiCaixa research centers have participated.
"It is a very interesting study that can partly explain why some older men have a worse prognosis," explains Manel Juan, immunologist at the Hospital Clínico de Barcelona.
"Now we will have to reconfirm these observations with more patients and, above all, study the presence of these antibodies over time," he adds.
The two jobs can help identify patients at higher risk for life-threatening pneumonia and even search for specific treatments for them.
Among them Rodríguez-Gallego points out two.
The immune system is a highly complex set of molecules with specialized functions: antibodies that neutralize viral particles, lymphocytes that identify infected cells and kill them, B cells capable of producing tens of thousands of antibodies, natural killer cells ... Among all of them there are three main types of interferons and, within type one, there are 17 different classes.
"If we find patients who produce antibodies against interferon alpha, which is a type of interferon 1, we could treat them with interferon beta, which is already used as a drug in other contexts," explains the immunologist.
The second option is to do a plasmapheresis: a filtering of the patient's blood to eliminate malignant antibodies and also other inflammatory molecules that may be making the disease worse.
You can follow
MATERIA
on
,
,
or subscribe here to our
newsletter
.