Developing, approving and manufacturing a vaccine is not straightforward - it
usually takes 10 to 15 years
, according to the Philadelphia College of Physicians.
However, the vaccine against SARS-CoV-2, which causes the disease COVID-19, was developed in a record time of less than a year.
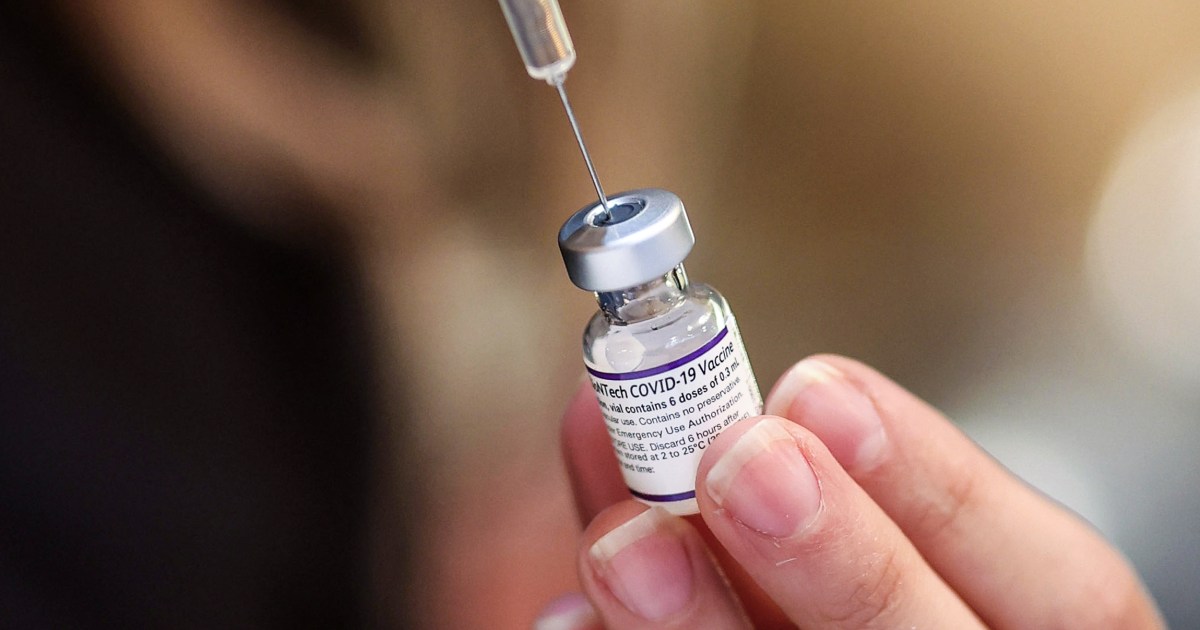
The Pfizer-developed vaccine is already being applied to front-line medical personnel in the United States, and millions of doses of Moderna's vaccine are already being distributed.
While this fast-paced scientific achievement might raise suspicions, the fact is that the COVID-19 pandemic sparked unprecedented global research cooperation.
To this is added that
research on the family of viruses called coronaviruses (named for their shape) was already well advanced,
since the
spike
protein
, used in the vaccine, had already been identified before by scientists.
[Follow our coverage of the coronavirus pandemic]
We explain how COVID-19 vaccines developed so quickly, and what stops drug companies from finding vaccines against diseases that for decades have killed hundreds of thousands of people, such as cancer and HIV.
Why is there no vaccine against cancer or HIV yet?
When we talk about cancer, it is important to keep two facts in mind: It is
generally not caused by a virus
, and no cancer has only one cause.
“Scientists believe that the interaction of many factors causes cancer.
The factors involve genetic, environmental and individual characteristics, ”explains Stanford University.
A historic day in Mexico with the start of vaccination against the coronavirus
Dec. 25, 202002: 14
Viruses such as
hepatitis B and human papilloma
viruses
can increase the risk of developing liver and cervical cancer, respectively.
Against them,
vaccines are already
available.
In contrast, there are no vaccines against bacteria that increase the risk of developing cancer, such as chlamydia or Helicobacter pylori.
Finding a vaccine against HIV, the human immunodeficiency virus, which causes AIDS, has not been easy because it
mutates rapidly and evades the immune system
, says the National Institute of Allergy and Infectious Diseases.
Injecting the inactivated or weakened virus, as is usually done with vaccines, has not been effective.
[No, coronavirus vaccines do not change DNA]
However, the pharmaceutical company Moderna is developing an HIV vaccine that uses messenger RNA (a single-stranded RNA molecule that complements one of the DNA strands), just like the coronavirus vaccine.
A vaccine from the Belgian pharmaceutical company Janssen has already reached phase 3, and will have clinical trials in Mexico, according to the newspaper El País.
Furthermore, HIV can be controlled thanks to antiretrovirals, which prevent AIDS from developing.
This treatment provides infected people with a life expectancy similar to the rest of the population.
Why were coronavirus vaccines developed so quickly?
The work to find a vaccine against COVID-19 did not start from scratch.
Research on hundreds of coronaviruses takes more than 50 years
, and scientists already knew of a structure, genome and life cycle similar to that of SARS-CoV-2, Dr. Eric told him.
J. Yager, professor of microbiology at the Albany University of Pharmacy and Health Sciences, to Medical News Today.
Coronaviruses cause common flu, as well as serious illnesses like MERS and SARS.
Just 10 days after the first cases were reported in Wuhan, China, researchers
discovered the genomic sequence
of SARS-Cov-2.
Confidence in COVID-19 Vaccine Grows: Up to 73% of Americans Would Get It
Dec. 26, 202000: 58
Unlike HIV, which is constantly mutating and has made it difficult to create a vaccine, SARS-Cov-2 is a relatively simple virus, whose mutations do not complicate vaccine development.
Another fundamental point to accelerate the vaccine was the
extraordinary financing
provided by the private and public sectors.
"The fact that governments bought vaccines in advance meant that people could take greater risks with [their research] at an earlier stage without having to go one step at a time," said Stephen Evans, professor of pharmacoepidemiology at the University. London School of Hygiene and Tropical Medicine.
COVID-19 vaccines are different
Vaccines usually consist of a weakened pathogen developed in a laboratory, which takes a long time to achieve.
But the vaccines that are being distributed, as well as those that are still in development, depend on the
protein s
pike
, which has simplified their development and manufacture.
More than a million people have already received the first dose of the vaccine in the United States
Dec. 23, 202000: 26
Messenger RNA vaccines contain material from the coronavirus that
provides the body's cells with instructions
on how to develop the
spike
protein
, which is unique to the coronavirus.
Once the cells make copies of that protein, the human body recognizes that the protein should not be there and builds T lymphocytes and B lymphocytes (types of white blood cells part of the immune system) that will
remember how to fight the virus that causes COVID- 19
if we become infected in the future, explains the Centers for Disease Control and Prevention (CDC).
With information from
Medical News Today
,
the Philadelphia University of Physicians
,
Stanford University
,
El País
,
CDC, Reuters.