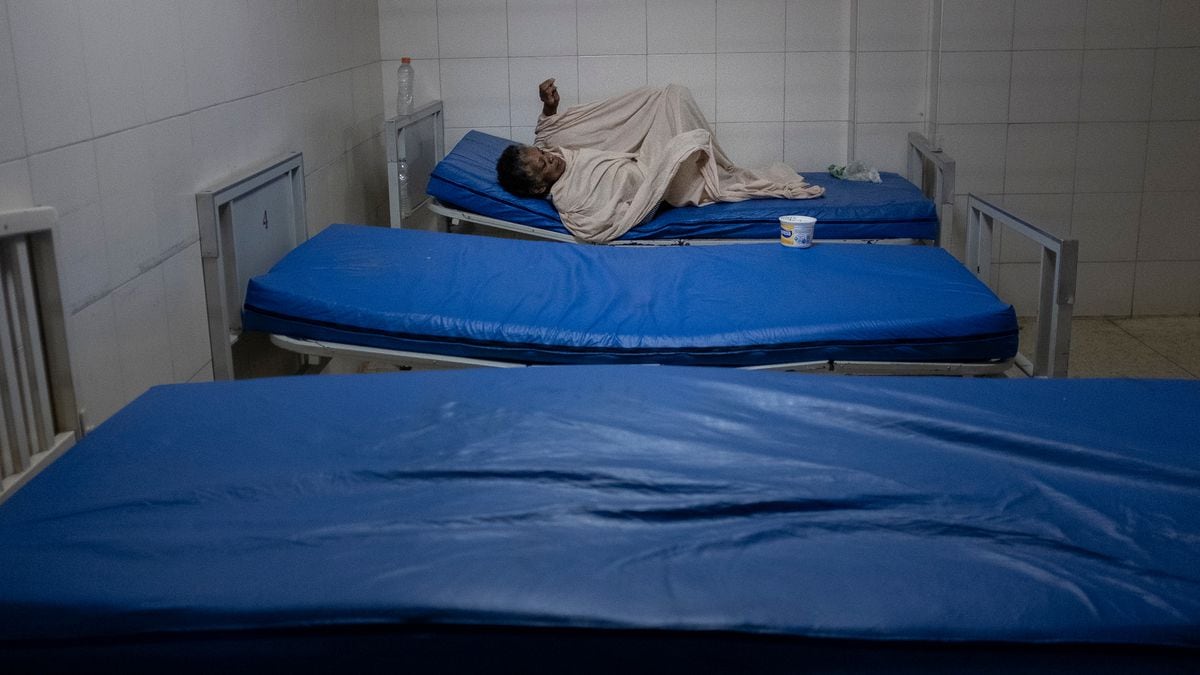
A mental health crisis: the other cost of the pandemic 5:22
(CNN) -
Americans are not getting the mental health care they need during the worst pandemic of the last century, according to the inaugural
"State of the Nation's Mental Health" report
released Monday by Anthem. , the largest for-profit healthcare company of the Blue Cross Blue Shield Association.
This is especially true in the case of the youngest, oldest and most impoverished, the groups most affected by illness, death and economic uncertainty caused by COVID-19, according to the report.
"Patient-reported rates of anxiety and depression increased, yet the ability to access mental health services decreased," said Dr. Shantanu Agrawal, Anthem Health Director.
Anthem's post follows a report released Friday by the U.S. Government Accountability Office (GAO) exploring the country's ability to access behavioral and mental health services during the pandemic. .
The GAO reported that 68% of the nearly 3,400 community clinics that serve low-income individuals with mental health and substance abuse issues had to cancel, reschedule, or reject patients in the past three months due to understaffing or Of funds.
"Our community clinics were already underfunded before the pandemic, so any reduction in revenue has an immediate effect," said Chuck Ingoglia, president and CEO of the National Council on Behavioral Health (NCBH). ), which represents many of the country's community clinics.
advertising
"Covid-19 has disproportionately affected low-income people, and these are the same people who are served by our member agencies," Ingoglia said.
"However, at the same time it has been more difficult for them to continue accessing their necessary mental health or substance abuse treatment."
The increase in alcohol consumption during the 4:36 pandemic
'The worst combination for mental health'
For more than a year, the pandemic has shaken the United States to the core, unleashing one devastating blow after another and cracking the very foundations of our lives - mentally, physically, and emotionally.
Add to this the stress of "a burgeoning alcohol and drug crisis ... deep structural problems related to social injustice in our country," we have "the worst mix for mental health needs," said Dr. Charles Marmar, chair of the department of psychiatry at NYU Langone Medical Center.
“There is a profound increase in the need for high-quality, accessible and equitable mental health care for all Americans.
There's no question about that, ”said Marmar, who also directs the Center for Alcohol Use Disorders and PTSD at New York University.
The warning signs of what Marmar calls a "wave of devastation" due to the mental health consequences of COVID-19 have been on the rise for some time.
Within two months of confinement in 2020, a Kaiser Family Foundation (KFF) survey found that worry or stress had led 56% of American adults to experience at least “one negative effect on their mental health and their health. well-being, such as problems sleeping or eating, increased alcohol consumption or worsening of chronic diseases.
Almost 41% of Americans were struggling with mental health problems stemming from the pandemic, such as depression, anxiety and suicidal thoughts, according to a survey by the US Centers for Disease Control and Prevention (CDC, for its acronym in English), held in June 2020.
In August of last year, the Commonwealth Fund analyzed mental health problems around the world and found that the US ranked first among nine nations, including Australia, Canada, France, Germany, the Netherlands, New Zealand, Sweden and the United Kingdom.
About 33% of American adults reported experiencing stress, anxiety, or great sadness that they found difficult to cope with alone.
Yet mental health care was the least accessible in the U.S. of the nine nations, according to the report.
During the pandemic, about 4 in 10 adults in the United States have reported symptoms of anxiety or depressive disorder, the Kaiser Family Foundation reported.
Young adults between the ages of 18 and 24 have been particularly affected: they are more likely to report substance use than all adults (25% versus 13%) and to have suicidal thoughts (26% versus 11%).
This organization serves the mental health of Hispanics 2:27
"Before the pandemic, young adults were already at high risk for mental health problems and substance use disorders, although many were not receiving treatment," the KFF report notes.
Anthem Report
The State of the Nation's Mental Health report is an analysis of the health insurance claims of 27 million members enrolled in Anthem's individual, employer-sponsored, Medicare and Medicaid health plans. in all 50 US states
The report found that diagnosis and treatment by mental health services were worse for children under 12 and adults over 75 than for other age groups.
The decrease was especially noticeable if the child or the elderly was a beneficiary of Medicare or Medicaid, which would occur in many of the economically disadvantaged areas most affected by COVID-19.
Children begin to present symptoms due to confinement by covid-19, says Save the Children
Older people used to have a difficult time using telehealth services that require video, even if they had a computer or smartphone at their disposal, which many do not, said clinical psychologist Vaile Wright, senior director of healthcare innovation. at the American Psychological Association.
"Older adults generally tend to prefer audio telehealth options, rather than video conferencing," Wright said.
“We really need audio-only visits to be covered by insurance;
in the future that is going to be really important for that population.
The children were in virtual schools, which eliminated individual observations by teachers who could detect signs of ADHD, behavior or adjustment problems, Agrawal said.
Virtual education affects children's mental health 0:45
"Teachers often make these initial, informal diagnoses and notify parents," Agrawal said.
"During the pandemic, these kinds of interactions happened much less, which meant that the children were probably not being diagnosed."
Even if a child is successfully diagnosed, the lack of specialized youth behavioral and mental health providers could hamper the child's ability to receive treatment, Wright said.
"We have a shortage of all mental and behavioral health providers in the country, and that is compounded when we talk about those who work with children," he added.
Treatment for Low Income and People of Color
A survey conducted in September 2020 among members of the National Council for Behavioral Health revealed that the demand for mental health services had increased greatly.
However, despite the need, the survey revealed that 26% of community clinics had laid off employees, 24% had laid off employees, and 43% had reduced work hours.
"On average, organizations have lost 22.6% of their income in the last three months during covid-19," the survey said, adding that "39% believe they will only be able to survive six months or less."
Another problem was obtaining personal protective equipment (PPE).
According to the September survey, a quarter of the clinics did not have enough PPE for two months.
How to feel good psychologically in the middle of the pandemic
Currently, federal aid to businesses, including the latest economic stimulus packages for COVID, is "certainly helping organizations get back to where they started," said Ingoglia of the NBCH.
But these are organizations that initially had few funds: when the covid arrived, they had to buy tablets and smartphones for both staff and some of their clients in order to continue providing their services.
"So getting back to the starting line is not going to be enough to accommodate the increased demand that we expect," Ingoglia said.
How to know if you need help
There are key signs you can look for, in yourself and your loved ones, that can indicate increased anxiety, depression, panic attacks, or possible suicidal behaviors.
Anxiety:
Having trouble concentrating, sleeping poorly, being restless and irritable are all signs that anxiety may be taking over your life in unhealthy ways, according to the American Psychological Association (APA).
Persistent or excessive worry about health or finances, often feeling overwhelmed by emotions, and a general feeling that something bad is going to happen are more signs.
Panic Attacks:
Sometimes anxiety can get out of control and lead to a full-fledged panic attack.
You may feel like you are having a heart attack - your heart rate may race or pound in your chest.
You may shake, sweat, feel like you're choking or short of breath, and feel scared.
These attacks can occur suddenly, without warning, and leave some people "fearful of when the next episode will occur, which can cause them to change or restrict their normal activities," notes the APA.
Irritability, a sign of depression in men 0:55
Depression:
Depression usually begins with a lack of energy and interest or pleasure in daily activities.
You may develop an inability to concentrate and feel worthless or guilty about an action or lack of it.
Paradoxically, you can experience significant weight loss or gain a lot of weight;
you can also sleep all the time or develop insomnia and sleep little.
You may even start thinking about death or suicide.
Signs of suicidal thoughts:
Often triggered by a recent loss through death, divorce, or separation, many of the signs that a person is at risk for suicide replicate those of depression and anxiety: loss of interest in friends or hobbies;
changes in sleeping patterns, eating habits, and personality;
low self-esteem, sadness, withdrawal, irritability, and feelings of guilt or worthlessness.
People at risk of suicide may start to behave erratically and talk about dying or hurting themselves.
According to the APA, they may show "no hope for the future, believing that things will never get better or that nothing will change."
What can you do for yourself
Choose healthy behaviors.
Instead of sitting on the couch, go outside and get some fresh air, sun, and exercise, experts suggest.
Exercise naturally creates endorphins, the body's wellness hormones.
Eating healthy, avoiding excess alcohol (a depressant), and getting enough sleep will also help your body… and your mind.
Come closer and speak.
"Create a space for dialogue," says Agrawal of Anthem.
"Ask your parents, your children, your spouse, your siblings: 'What was it like going through this pandemic?'"
By having those conversations, you can work to uncover mental health issues that might not have otherwise been noticed, he said.
"And when you discover these problems, offer support to your family member, but also help them get that professional support if they need it," Agrawal said.
"That can go a long way toward addressing stigma, and not discovering the problem and then trying to cover it up."
Seek support.
Look for federal, state, and local resources.
If the situation is life threatening, seek immediate emergency help by calling 911. If it is not, start with the distress help lines.
The Substance Abuse and Mental Health Services Administration, or SAMHSA, has a national helpline 800-662-HELP (4357) that provides free and confidential treatment information and referrals in English and Spanish, 24 hours a day, every day of the year.
The American Psychological Association also has a Suicide, Substance Abuse, and Domestic Violence Resource Webpage.
Don't wait for a crisis to find help, says Reginald Williams, vice president for International Health Policy and Practical Innovations at the Commonwealth Fund, which works to promote equity in America's health care.
"There are hotlines called 'warm lines' that people can go to and voice their concerns, express their frustrations and they can get in touch with services and resources to help them," Williams said.
Mental Health America has a 'warm lines' website in states across the country.
"These lines are generally a direct line run by people who provide support to those who may have some sadness, some pain, feel a little overwhelmed, but are not thinking of harming themselves or others," Williams said.
Seek ongoing therapy.
If you have health insurance or other resources, try to find a therapist.
Most clinics and therapists offer visits by phone or video.
Many employers are offering free access to therapists as part of their employee benefit plans, and many communities have tiered fee mental health centers.
Marmar of New York University suggests calling the intake line for the psychiatric outpatient clinic at the nearest medical school.
“The social and intake workers there know all the regional resources.
It always works, and the best thing is that you get a quality referral, "says Marmar.
Many people choose not to go to therapy, according to experts, because they think it makes them "weak" or seems too invasive.
But that's not the therapy, Eve Byrd, director of the Carter Center's Mental Health Program, said in an earlier interview with CNN.
"Therapy is really an educational activity."
The role of a therapist is "to help think about different ways of reacting to situations" and "more positive ways of interacting with people," he said.
It's okay not to be okay sometimes.
In a way, our national tension over a deadly virus has brought us together, and makes us aware of how fragile we can be, both in body and in mind.
"Certainly, I would have preferred not to have a pandemic to really understand the priority of our mental health and well-being," Wright said.
- CNN's Kristen Rogers and Naomi Thomas contributed to this report.
Covid-19 Mental Health