Carl zimmer
05/06/2021 13:05
Clarín.com
The New York Times International Weekly
Updated 05/06/2021 13:05
In early 2020, dozens of scientific teams rushed to make a vaccine against COVID-19.
Some chose proven techniques, such as making vaccines from killed viruses.
But a handful of companies opted for a riskier approach, which had never produced a licensed vaccine: using a
genetic
molecule
called RNA
.
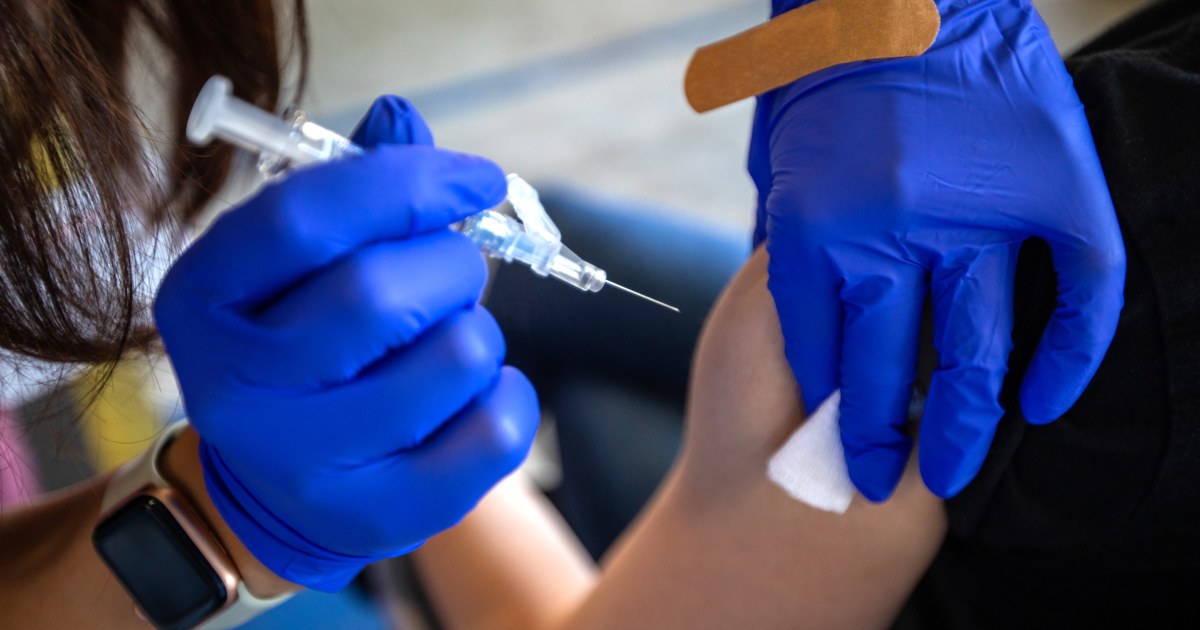
A volunteer receives a dose of the CureVac vaccine or a placebo.
Photo REUTERS / Yves Herman / File Photo
The bet paid off.
The first two vaccines to successfully
emerge
from clinical trials, made by
Pfizer-BioNTech
and
Moderna
, were made from RNA.
Both turned out to have
the best efficacy rates
that a vaccine can have.
In the months that followed, those two RNA vaccines have provided protection to tens of millions of people in about 90 countries.
But many parts of the world, including those with a growing death toll, have had
little access
to them, in part because they
need to be kept in a freezer.
Now, a
third RNA vaccine
can help meet that global need.
A small German company called
CureVac
is about to announce the results of its late-stage clinical trial.
As early as next
week
, the world could know if your vaccine is safe and effective.
CureVac's product belongs to what many scientists call the
second wave
of COVID-19 vaccines, which could collectively alleviate global demand.
It is expected to
Novavax,
a company based in Maryland whose coronavirus vaccine uses proteins, request the US approval in the coming weeks.
Tests
In India, the pharmaceutical company
Biological E
is testing another protein-based vaccine that was developed by researchers in Texas.
In
Brazil, Mexico, Thailand and Vietnam
, researchers are beginning trials of a COVID-19 vaccine that can be mass-produced in chicken eggs.
Vaccine experts are especially curious to see the results of CureVac because its injection has a
significant advantage
over other RNA vaccines from Moderna and Pfizer-BioNTech.
While those two vaccines have to be stored in a freezer, CureVac's is stable in a refrigerator, meaning it could more easily bring the newfound power of RNA vaccines to the worst affected areas of the world.
"It has gone largely unnoticed," said Jacob Kirkegaard, a researcher at the Peterson Institute for International Economics in Washington, DC But now, he added, "it seems to be very well positioned to reach the world market."
For CureVac co-founder biologist
Ingmar Hoerr,
the company's COVID-19 vaccine trial is the culmination of a quarter-century of work with RNA, a molecule that helps convert DNA into the proteins that make the work of our cells.
As a graduate student at the
University of Tübingen
in the 1990s, Hoerr injected RNA into mice and discovered that the animals could
manufacture the protein encoded
by the molecules.
He was surprised to find that the immune systems of the mice produced antibodies against the new proteins.
Hoerr thought it could be the basis for a new type of vaccine.
"I thought, 'Wow, if this works like that in humans, then we have a completely new pharmaceutical possibility,'" he said.
At the time, only a few scientists in the world considered an RNA vaccine to be a serious possibility.
But its advocates thought it could change medicine.
In theory, an RNA molecule could be created to immunize people
against any virus.
You could even create an RNA vaccine to
cure cancer
, if you could make an RNA molecule that encodes a tumor protein.
In 2001, Hoerr co-founded CureVac to pursue that idea, but for the first few years the company struggled
to survive
.
To stay on his feet, he received orders from other labs for custom-made RNA molecules.
On the other hand, the CureVac scientists experimented with their own RNA vaccine designs.
Over time, they found
subtle adjustments
to the RNA vaccine molecules that caused the cells to make
more proteins.
The more potent the RNA, the lower the dose required in vaccines.
The CureVac researchers also discovered how to put RNA molecules
in bubbles of fat
to protect them from destruction on their way into cells.
And perhaps most importantly, they used a form of RNA that could remain stable in relatively warm temperatures.
Instead of needing a freezer, the CureVac vaccine could be refrigerated.
Over time, other companies also entered the RNA vaccine business: BioNTech in Germany in 2008, and then Moderna in Boston in 2011.
His experiments began to show that these vaccines could protect animals against a wide variety of viruses.
In 2013, CureVac injected
human volunteers with
an RNA vaccine against
rabies,
in the
first clinical trial
of this technology against an infectious disease.
For years, CureVac and other RNA vaccine companies struggled to perfect their vaccines.
CureVac's first attempt at creating a rabies vaccine proved it to be safe, but gave a
weak
immune system
response
.
Since then, the company has modified that vaccine, and the updated version has shown
promise
in early clinical studies.
But other efforts ended in failure.
In 2017, CureVac announced that its RNA prostate cancer vaccine offered no benefit to patients.
Despite these setbacks, the company built a
solid reputation
.
"They ticked the boxes for scientific acumen, speed, scale and access," said Nicholas Jackson, head of programs and innovative technology at the
Coalition for Epidemic Preparedness Innovations
, a foundation that supports vaccine research.
CEPI gave
CureVac
$ 34 million
in 2019 to support its development of RNA vaccines for future pandemics.
When the coronavirus pandemic struck, CureVac, BioNTech, and Moderna set out to make RNA vaccines.
But BionTech and Moderna soon take the lead thanks in part to allies
with a
lot of
money
.
BioNTec
h partnered with the pharmaceutical giant
Pfizer,
while Moderna worked with the
National Institutes of Health
and received
$ 1 billion from the US
government as part of
Operation Warp Speed
.
CureVac was left behind.
CEPI provided the company
with $ 15 million
, but CureVac would need much more.
"If you do this, you need a considerable amount of cash," Franz-Werner Haas, CureVac's chief executive officer, said in an interview.
"And the considerable amount of cash was not there."
In March 2020, German newspapers reported that former President
Donald Trump
had offered CureVac $ 1 billion to move its operations to the United States.
CureVac denied the reports, but the CEO suddenly left, to be replaced by Haas.
The CureVac researchers went ahead with their limited resources, designing an RNA molecule that encodes a protein found on the surface of the coronavirus, called a spike.
The
experiments with hamsters
showed that could protect animals from the virus.
In June, the
German government
invested 300 million euros (about $ 360 million) in CureVac's research on COVID-19, and other investors soon followed.
In December, after promising data from the first safety studies, the company began its latest trial, called
phase three
, in which 40,000 volunteers were recruited in Europe and Latin America.
The company will obtain its first data when
56 volunteers develop COVID-19.
If most of them are in the placebo group and few are in the vaccinated group, it will be proof that the vaccine works.
Haas said it expected to have that data by mid-May.
There is no way of knowing in advance how CureVac will fare.
But given the performance of other RNA vaccines, coupled with the early results from CureVac, some scientists have
high expectations.
"I would be very surprised if it didn't work well," says John Moore, a virus expert at Weill Cornell Medicine in New York, who has collaborated with CureVac on an RNA-based HIV vaccine.
Competence
Still, the CureVac vaccine faces a challenge that Pfizer and Moderna did not have:
new variants
that may be able to attenuate its efficacy.
Experiments in mice have suggested that the vaccine works well against the
B.1.351
variant
, which first appeared in
South Africa
.
Last year, CureVac partnered with several large companies to
increase production
of its COVID vaccine should its clinical trials prove successful.
The company also negotiated a deal with the European Union for
225 million doses
, as well as an option to add another 180 million doses in the following months.
But now it's unclear who could get the CureVac vaccine if it becomes available next month.
In January, the
European Union
gave emergency authorization to an
AstraZeneca
vaccine
,
with the intention of relying on that company for most of the supply.
But AstraZeneca failed to deliver on its supply promises, prompting the bloc to
retaliate with a lawsuit.
In April, the European Union finally fixed this shortfall, negotiating
with Pfizer and BioNTech
to obtain 1.8 billion doses of its vaccine by 2023.
That deal has left analysts wondering
how much demand
will be left for CureVac.
"They're going to miss out on the major markets in the advanced economy," Kirkegaard said.
"The United States, Europe and Japan are going to be vaccinated heavily with these Moderna and Pfizer vaccines."
Haas countered that most of the doses from the Pfizer-BioNTech block will not arrive until next year.
"CureVac sees itself as a
major player
in ending the COVID-19 pandemic in Europe and elsewhere," he said.
But CureVac will also have to cope with a
global shortage of the raw materials
needed for RNA vaccines.
The shortage is especially dire for the company because imports from the United States are
limited
by the
Defense Production Act
.
Unlike Pfizer-BioNTech or Moderna, CureVac does not have facilities in the United States.
"The US Defense Production Act has been a factor affecting our access to some materials and supplies," Haas said.
"However, we currently do not expect it to substantially influence our manufacturing forecasts for the remainder of 2021 and beyond."
Ursula von der Leyen,
president of the European Commission, said that if the CureVac vaccine worked, it would be on the list, thanks to two advantages: It is an mRNA vaccine, and it was
created in Europe.
It is also possible that some European countries reach parallel agreements with the company.
Billions of other people in low- and middle-income countries have yet to receive a vaccine, and experts say CureVac could meet some of their demand.
"
We continue to need many vaccines
around the world," says Florian Krammer, a virus expert at the Icahn Mount Sinai School of Medicine in New York.
"I think a lot of people can benefit from it."
Moderna and Pfizer-BioNTech vaccines are
difficult to distribute
in the developing world due to the equipment and power supply required to freeze these vaccines.
The CureVac RNA vaccine can remain stable for at least
three months
at 5 degrees and can remain
24 hours at room temperature
before being used.
"Stability is a real advantage," Jackson said.
CEPI is "in very active discussions" with CureVac, he said, about distributing the company's vaccine through Covax, an initiative to distribute vaccines to
low- and middle-income countries.
But CureVac is also designing a new generation of vaccines with the goal of reaching markets in the United States and other wealthy countries.
Since its powerful RNA only requires a small dose, the company could create vaccines for
different variants and mix them in a single injection.
But these possibilities don't make sense until CureVac can show that their vaccine works.
Mary Warrell, a vaccine researcher at the
University of Oxford
, is reluctant to speculate on the fate of the vaccine before that milestone.
"Prediction during this pandemic has rarely been profitable," he warned.
Matina Stevis-Gridneff contributed a feature story.
c.2021 The New York Times Company
Look also
How Europe sealed a deal with Pfizer with texts and calls
Rich countries gave up in writing the chance to vaccinate the world