Anita Banda flashes a small smile as she looks at the toy pelican she is holding in her hands.
“I already wanted to go home.
My other children and my grandchildren need me,” says her mother, Cristine Chapoda, 45.
Just a week ago, she and Anita, her youngest daughter, barely two and a half years old and with a small and delicate body, arrived at the pediatric unit of the Central Hospital of Kamuzu, in Lilongwe, the capital of Malawi, because the girl had a fever And cough.
“She came with acute malnutrition.
We also tested her for tuberculosis and she was positive.
And she also has HIV, ”says Nora Ferrer, the 29-year-old Spanish pediatrician who has treated her.
For now, she no longer has to worry about the first two diagnoses.
Hence, mother and baby prepare to leave the center.
The fight against the third will last a lifetime.
“I don't have a job;
I dedicate myself to my house and my children.
They are four.
And also two grandchildren”, explains Cristine, who, with so many children, already has experience in hospitals and pediatricians.
“I had already been here three times before.
First, with my eldest son, who is asthmatic.
Another once fell ill with pneumonia.
And with Anita I also came recently, ”she says.
For Cristine, who lives in Lilongwe, going to the doctor is a short two-hour bus ride, although the distance could be worse.
The Kamuzu is a referral hospital for seven million people (the capital city barely reaches one million) and has one of the largest pediatric departments in Africa, with some 250 beds and around 24,000 admissions of children a year.
Nor is this figure surprising in such a young nation: 43% of the country's population,
A unit of the pediatric department of the Kamuzu Hospital, where the beds are shared by three or four children and their mothers.José Ignacio Martínez Rodríguez
However, at a glance, those 250 beds seem insufficient.
In most of the rooms and pavilions that make up the pediatric unit, children share mattresses with their mothers and with other patients.
Up to five little ones in some of them.
Cries, laughter, screams are heard.
The bustle of people through the corridors (doctors who go, nurses who come, patients who complain or ask questions and relatives who bring the lunch of the day) is constant.
“The mothers have the singing voice here;
They are the ones who almost always accompany their children and some come from far away,” says Irene Alcázar, the 28-year-old nurse who has treated Anita with Ferrer.
And she adds: “Everything here is a little more difficult.
Sometimes, for example, samples are lost, which greatly delays diagnoses,
Ferrer and Alcázar, who work for two months at the Kamuzu Central Hospital along with five other Spanish health workers with the Malawi-Health Association NGO, with more than a decade of experience in this center, comment on other day-to-day difficulties.
“There are times when, when you want to consult a specialist doctor, you have to send him a WhatsApp.
Everything is more informal”, indicates the nurse.
“One of the first days we wanted to revive a child, but we had no adrenaline.
So what I do now is always carry a dose in my pocket”, adds Ferrer.
And she shows the little glass jar that she keeps like a treasure.
She looks at him and they both smile.
“Sometimes you feel helpless…”, they say.
And they also speak of the scarcity and need of families.
“You notice it in little ones who, although they are healthy, suffer from malnutrition.”
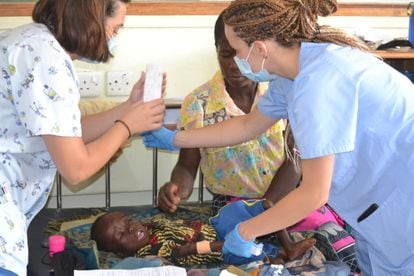
Nora Ferrer and Irene Alcázar, a Spanish pediatrician and nurse, treat a girl who has arrived at the hospital with signs of malnutrition.José Ignacio Martínez Rodríguez
Poverty, implacable enemy
Malawi makes a notable effort on paper in terms of health, since its health system, to which it spends more than 7% of its GDP, is public and free (other surrounding states, such as Tanzania or, further north, Kenya, charge for many of the medical services they provide), and that is one of the poorest countries in the world: 50.7% of its population lives below the poverty line, according to the United Nations Development Program (UNDP ).
This organization places it in position 171 of its Human Development Index, a list that includes 189 nations.
People like Binallson Moyo, a 32-year-old man who has gone to the hospital with his son Moses, a five-year-old albino boy, put a face to this stark statistic.
"I can't buy you everything you need"
summarizes in front of the bed where her child hopes to recover from a disease that affects his skin.
“I came on Monday, but I still don't know what's wrong with him.
Nor how long are we going to have to stay here.
Although I have been told that he is going to get well, ”she celebrates in broken English.
In an adjoining room, Alice Nyiramuyisha, a 36-year-old Congolese woman, holds her 10-month-old daughter Icramina in her arms.
She does so sitting on the floor next to their assigned bed.
"She has a heart problem and has tested positive for tuberculosis," laments her mother.
Icramina also has Down syndrome.
Alice lives in Dzaleka, a refugee camp located about 40 kilometers from Lilongwe.
She arrived there seven years ago now fleeing from the conflicts in her country and there she continues with her 10-month-old baby and her other four children.
“We subsist on the food provided by UNHCR [the UN refugee agency].
But the situation is disastrous.
When we get sick they only give us pills for the head.
Here, at least, I have everything my girl needs, ”she celebrates.
And she also says that she already knows the way and the center well,
Moses, a boy with albinism, sits on a bed in the pediatric unit at Kamuzu Central Hospital in Lilongwe, Malawi.
He arrived suffering from a skin disease.José Ignacio Martínez Rodríguez
“The calf has had a pericardial effusion.
It is not normal, although heart disease may be more common due to a Down history.
She had already been hospitalized three months before in a frankly bad state, ”explains Estibaliz Badiola, the 30-year-old pediatrician who cares for Icramina.
And she continues: “Alice and the other parents have to go to another building to get the tuberculosis medicine at five in the morning.
If they arrive at half past five, they are left without treatment.”
And not having medicines for this disease, the deadliest infectious disease on the planet until the arrival of covid-19, can lead to drama.
Not in vain, the deaths caused by this pathology approached one and a half million in 2020 throughout the planet.
The World Health Organization also indicates that 25% of these deaths occur in African countries.
“This girl would be in the ICU, with control and continuous monitoring.
Here there are times when we cannot know if what the kids have is contagious or not, even if four or five of them share a bed,” says Patricia González, the 33-year-old nurse who, together with Badiola, is in charge of caring for Icramina.
“There is no scanner right now and microscopic tests are not always accepted;
we may have a patient without knowing if she suffers from a simple virus, tuberculosis or something tumorous, ”she says.
And, finally, she indicates that the pathologies that are most treated in the hospital's pediatric unit are bronchiolitis, pneumonia and malaria, diseases to which mothers and children in Malawi have become accustomed by force.
Some overcome them without difficulty.
On the other hand, others are too deadly.
Admissions, recoveries and deaths
Joyce Chilonga is 22 years old and has two children.
The youngest, Blessings, a few weeks old, started sneezing and running a fever a few days ago, so Joyce carried him on her back, caught a bus, and took him to the hospital.
“Since I came, my baby has improved a lot.
Today they told me that we can go home,” says the young mother.
“The child had bronchiolitis.
Respiratory infections are usually the most frequent reason for admitting infants.
It's quite normal.
Also in Spain”, says Alejandro Jiménez, the 29-year-old doctor who has been in charge of the Blessings case.
“But there are differences, of course.
You have a kid who enters Spain for this all the time connected to a heart rate monitor.
Here he often depends on what the mother may think, ”he explains with a half smile.
Carla Barcelo,
the 29-year-old nurse who has accompanied him with this patient, listens and adds: “And there are specific pediatrics.
Here we use those of adults for children too”.
Cristine and her daughter Anita, who arrived in Kamuzu with severe malnutrition and tuberculosis, are discharged and prepare to return home.José Ignacio Martínez Rodríguez
However, these respiratory infections usually have a happy ending and only rarely lead to the death of the patient, a reality that the pediatricians who work at the Kamuzu center must deal with almost daily.
An extensive report published in 2018 by BMC Pediatrics titled
An audit of pediatric deaths in a large referral hospital in Malawi
put real figures to this painful situation.
In the 13 months that the study lasted, the center registered 743 deaths in this unit, an average of two per day.
Malaria, which caused 183 deaths in this period (26.1%), malnutrition, with 95 (13.6%), and complications from HIV, with 69 (9.9%), were the three main causes of such a sad statistic.
Despite this, said letter also includes reasons for optimism.
"The mortality rate, while still high, has dropped here dramatically in the six years since the last published mortality data," he concludes.
“This is like an obstacle course.
It's hard to get used to the fact that nothing is computerized.
Or that the power suddenly goes out and all the machines turn off”, summarizes Barceló.
“I have had a case of a one-year-old boy, a very smart boy, who had a non-complex cardiac malformation.
He could be operated on and would lead a normal life, but here, he will probably die in a few months or, like many, in a few years, ”says Jiménez.
And both also comment on the high frequency with which antibiotics are given to children, which makes them more resistant to bacteria, or the difficulty of obtaining medicines at the pharmacy, or of carrying out diagnostic tests... "We can treat three or four children a day”, they conclude.
But the work in pediatrics in such challenging circumstances, looking at some past examples,
From the incubator, to a pediatrician
“My mother told me that I was premature.
I had to be in an incubator for a few days and there were people who worried about me.
Although I was at risk of dying, someone took their time to take care of me.
I became a pediatrician for that;
now I can be part of the team that saves a child,” says Yewo, a 32-year-old Malawian pediatrician who works side by side with the Spanish team.
“The challenges here are constant because people have a lot of problems and our resources are very limited.
Most of the patients have to come on their own and sometimes we lose them because they don't come in time to heal,” he explains.
And he also affirms that the local staff that makes up the unit are six doctors and eight clinical officers – a health worker with three years of training instructed to deal with the most common diseases.
Yewo, a Malawian pediatrician, attends to some patients and their mothers at the Kamuzu Hospital.José Ignacio Martínez Rodríguez
This Malawian pediatrician tells that he studied medicine in his native country, that when he finished it he joined the pediatric department of the Kamuzu Central Hospital and that, in 2012, he was awarded a scholarship to further his studies and knowledge in Cuba.
When he returned in 2019, he rejoined the unit he already knew.
And, since then, it has been fighting daily so that hundreds of children can overcome malaria, severe malnutrition or lead a decent life as HIV carriers, something really complicated in a country where 70% of deaths in hospitals are caused by HIV. AIDS virus.
Yewo concludes: “Sometimes it's a tough job, but it pays off.
When a child recovers… I don't know, it's like a process that you can see perfectly.
I think that's the best thing about our job."
You can follow PLANETA FUTURO on
,
and
, and subscribe
to our 'newsletter'
here
.